Building a family does not always follow a straight path, and for millions of people around the world, an at home insemination kit has become one of the most practical, private, and emotionally empowering options available today. Whether you are a single woman using donor sperm, an LGBTQ+ couple building your family, or a heterosexual couple navigating timing challenges or mild male-factor infertility, understanding how home insemination works can genuinely change the trajectory of your fertility journey.
This guide breaks down everything — what an at home insemination kit actually contains, how the process works step by step, the real success rates backed by research, common mistakes that reduce your chances, and exactly how to optimize every cycle. No vague promises, no recycled clinic brochure language — just a clear, practical, and complete picture of what this process involves.
What Is an At Home Insemination Kit and Who Uses It
An at home insemination kit is a collection of medical-grade tools that allows you to perform intracervical insemination (ICI) in the comfort and privacy of your own home. The process involves introducing sperm into the vaginal canal near the cervix without sexual intercourse, using a specially designed syringe rather than any invasive clinical procedure.
The method is also referred to as intracervical insemination at home or intravaginal insemination (IVI), and it sits at the more accessible end of the assisted reproductive technology spectrum. It does not involve injecting sperm directly into the uterus the way clinical IUI does — instead, sperm is deposited near the cervical opening, allowing it to travel naturally through the cervix and into the uterus.
People who typically use a home insemination kit for couples or individuals include:
- Same-sex female couples using donor sperm from a licensed sperm bank
- Single women who have chosen to conceive independently
- Heterosexual couples where intercourse has become stressful due to performance anxiety tied to fertility pressure
- Couples dealing with mild low sperm count where concentrating delivery improves chances
- Couples who find clinical settings emotionally difficult or financially out of reach
Artificial insemination at home has grown significantly in visibility over the past decade, driven by better product design, increasing FDA oversight, and greater cultural openness about diverse paths to parenthood.
What Does an At Home Insemination Kit Contain
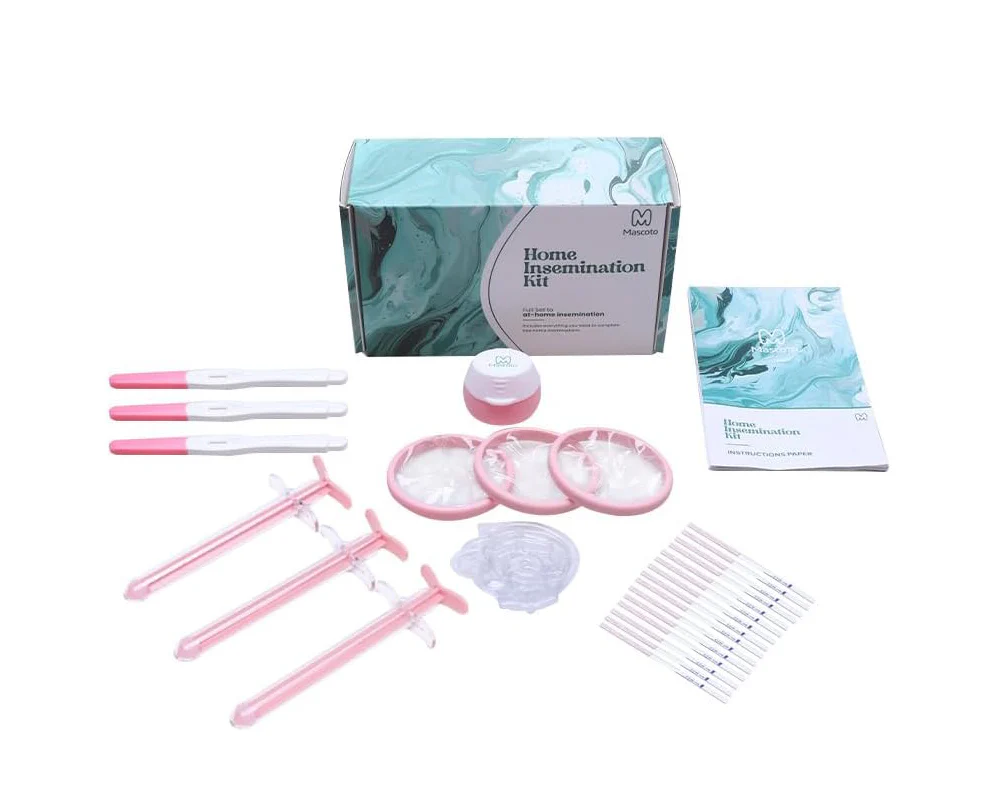
Most kits are designed to include everything needed for one or two complete insemination attempts. A standard at home insemination kit typically contains:
Insemination syringe — The core component. Modern kits use a soft-tipped, needle-free syringe specifically engineered for the vaginal canal. Some feature patented slit-tip openings designed to deliver a wider, deeper spray near the cervical opening. The tip is rounded and smooth for comfort, and it is made from body-safe, BPA-free medical-grade materials.
Sperm collection cup — A sterile, rounded container used for sample collection before transferring the sperm into the syringe. The cup and syringe are designed to work together to minimize waste and maximize transfer.
Ovulation predictor test strips — Many complete kits include these to help you pinpoint your fertile window using LH surge detection. Knowing your exact ovulation timing is the single biggest factor in whether insemination is successful.
Cervical disc or soft cervical cap (in some kits) — An optional component designed to hold the sperm sample in place against the cervix after insertion, reducing leakage and extending contact time.
Sperm-friendly lubricant — Included in premium kits because standard vaginal lubricants are toxic to sperm and can reduce sperm motility by nearly 50%. Only lubricants specifically formulated to be sperm-compatible should be used around insemination.
Step-by-step instructions — Clear guidance on timing, positioning, sample handling, and what to expect during and after the process.
Components should all be sterile, individually packaged, and ready to use directly from the box. Washing components with water or soap before use can actually harm sperm — the packaging is already clean-room prepared for immediate use.
How to Use an At Home Insemination Kit — Step by Step
Using an at home insemination kit properly is not complicated, but every step matters. Getting the timing right, handling the sample correctly, and positioning yourself well all directly affect your chances of home insemination success rate improving over multiple cycles.
Step 1 — Track Ovulation Precisely
Timing is the most critical variable in the entire process. The egg survives only 12 to 24 hours after ovulation, so insemination must happen within that narrow window.
Use ovulation predictor kits (OPKs) to detect your LH surge — the hormonal spike that occurs 24 to 36 hours before ovulation. Begin testing from around day 10 of your cycle, counting from the first day of your period. Test at the same time each day, ideally mid-morning.
Combine OPK testing with monitoring cervical mucus changes — as you approach ovulation, cervical mucus becomes clear and stretchy, resembling raw egg whites. This is your body signaling peak fertility.
Some women also use basal body temperature (BBT) charting as a secondary confirmation tool. BBT rises slightly after ovulation, which confirms it occurred, though it cannot predict it in advance the way OPKs do.
Step 2 — Prepare the Sperm Sample
If you are using a partner’s sperm, the male partner should avoid ejaculating for one to three days before collection to maximize sperm count and quality. A longer abstinence period beyond three days can actually reduce motility, so the one-to-three-day window is optimal.
For at home insemination kit insemination with donor sperm, follow the thawing instructions provided by your sperm bank precisely. Frozen donor sperm typically arrives in a liquid nitrogen tank and must be thawed at room temperature or under specific conditions. Once thawed, frozen sperm is viable for approximately 12 to 24 hours. Fresh sperm from a partner remains viable for up to 72 hours.
Once the sample is collected or thawed, inseminate as quickly as possible. Sperm is most viable within the first 30 minutes of collection.
Step 3 — Draw the Sample Into the Syringe
Open the sterile syringe from its packaging. Draw the sperm sample slowly into the syringe by pulling back the plunger while the tip is submerged in the sample. Avoid drawing in air. If air bubbles appear, point the syringe upward and gently tap it, then push the plunger slightly until bubbles clear and the sample reaches the tip.
Do not shake the syringe vigorously — gentle handling preserves sperm integrity.
Step 4 — Position Yourself Correctly
The best position for home insemination is lying on your back with your hips elevated on a firm pillow. This uses gravity to help the sperm travel toward the cervix rather than leak out. Some people also find lying on their side comfortable while maintaining elevated hips.
Insert the syringe gently into the vaginal canal. You do not need to locate the cervix manually — the goal is to deposit the sample as close to it as possible, not inside it. Depress the plunger slowly and steadily to release the sample.
Step 5 — Remain Still for 20 to 30 Minutes
After insemination, remain in the same position — on your back with hips elevated — for at least 20 to 30 minutes. This allows the sperm to travel toward the cervix and reduces the amount that exits through leakage. It is completely normal to notice some fluid leaking afterward, as semen fluid naturally exits the body once its carrier function is complete.
Use the bathroom before you begin the insemination process, not after, and wait at least 30 minutes post-insemination before urinating.
Step 6 — Repeat Within the Same Cycle
Inseminating twice per cycle — once at the first positive OPK result and again 12 to 24 hours later — is consistently associated with higher success rates than a single attempt. This accounts for variation in the exact moment of ovulation and gives sperm the best chance of meeting the egg within its viable window.
At Home Insemination Success Rate — What the Data Actually Shows
One of the most searched questions around this topic is what the real home insemination success rate looks like. The honest answer is that it varies considerably depending on age, sperm quality, timing accuracy, and underlying fertility factors — but the numbers are more encouraging than most people expect.
Per-cycle success rates for the intracervical at home insemination kit average between 10% and 20% for women under 35. For women under 35 with no identified fertility issues and correctly timed insemination, the per-cycle rate sits around 18 to 20%. This means roughly 1 in 5 well-executed attempts results in pregnancy.
However, cumulative success rates tell a more complete story. Over six well-timed cycles, many people with no underlying fertility issues will achieve conception. A 2021 study found that individuals who participated in at home insemination kit had a cumulative success rate exceeding 40% across multiple cycles, making it a genuinely effective option when approached with consistency.
Key factors that directly influence your success rate include:
- Timing accuracy — Off-cycle insemination is the most common reason for failure, not kit quality
- Age — Success rates decline as age increases, particularly after 35
- Sperm quality — Fresh sperm from a partner generally outperforms frozen donor sperm per cycle, though both are valid options
- Number of inseminations per cycle — Two attempts per cycle significantly outperform one
- Underlying fertility conditions — Undiagnosed ovulatory disorders or blocked fallopian tubes will limit results regardless of technique
Choosing the Right At Home Insemination Kit for Your Situation
Not all kits are built equally, and the right at home insemination kit depends on your specific circumstances.
For couples using partner sperm — Look for kits that include a collection cup designed to work seamlessly with the syringe, minimizing transfer waste. Kits with two attempts included per package allow you to inseminate twice per cycle without purchasing extra supplies.
For single women or LGBTQ+ couples using donor sperm — Frozen donor sperm arrives in small volumes, so choose a kit specifically designed for low-volume samples. The collection cup shape matters here — rounded cups that allow the syringe tip to reach the bottom reduce waste considerably.
For those with low sperm count or motility concerns — Some kits include a cervical disc or soft cap that holds the sample against the cervix for several hours after insemination, extending contact time and improving the chances of fertilization.
FDA clearance — This is an important consideration when evaluating kits. In recent years, FDA clearance has become the standard requirement for devices used in at-home insemination. An FDA-cleared kit has been evaluated for substantial equivalence to devices used in clinical settings and offers a level of quality assurance that unregulated products do not provide.
Material safety — Confirm the kit uses BPA-free, medical-grade, body-safe materials. Avoid any kit that does not specify the material composition of its syringe and collection components.
Reusable vs. single-use — Some kits are designed for single-use sterility, while others are reusable with proper sterilization between cycles. Consider your expected number of cycles and total cost when evaluating which format is more economical for your situation.
at home insemination kit With Donor Sperm — What You Need to Know
at home insemination kit with donor sperm is one of the most common applications of these kits, particularly for single women and same-sex female couples. The process requires a few additional steps and considerations beyond using a partner’s sample.
Donor sperm should always be sourced from an FDA-registered sperm bank that follows established screening protocols for infectious diseases, genetic conditions, and sperm quality. Purchasing from unregulated sources or private donors outside a licensed bank introduces significant medical and legal risks that are not present with properly screened cryopreserved donor sperm.
When you order from a licensed sperm bank, the vials are shipped in a liquid nitrogen storage tank directly to your home. Handling and thawing instructions are included and must be followed precisely. After thawing, the sperm should be brought to room temperature and used within the timeframe specified — typically within one to two hours.
From a legal standpoint, using a sperm bank provides clear documentation of donor identity, consent, and parental rights separation. Private donor arrangements without proper legal agreements can create complex and emotionally difficult disputes around parental rights in the future. This is an area where consulting a reproductive law specialist before proceeding is genuinely worth the effort.
Common Mistakes That Reduce Your Chances
Understanding what reduces the home insemination success rate is just as important as knowing what increases it.
Using lubricants not designed for insemination — Standard vaginal lubricants and even many water-based lubricants reduce sperm motility significantly. Only use lubricants that explicitly state they are sperm-compatible.
Inseminating too early or too late in the cycle — Guessing your ovulation window rather than using OPKs is the most preventable source of failed cycles. Invest in quality ovulation predictor strips and test consistently.
Vigorous handling of the sperm sample — Shaking the vial or syringe damages sperm. Swirl gently and handle with care throughout the process.
Getting up immediately after insemination — Standing up immediately after the procedure allows gravity to work against you. The 20-to-30-minute rest period is not optional if you want to give the sample the best chance of reaching the cervix.
Using non-sterile equipment or improvised tools — at home insemination kit syringes, unsterilized containers, or equipment not designed for insemination introduce infection risk and can compromise the sample. Use only purpose-built, sterile kit components.
Ignoring lifestyle factors — Strenuous exercise immediately before and after insemination can interfere with implantation. Alcohol, smoking, and excessive caffeine have documented negative effects on fertility. Prenatal vitamins including folic acid, iron, and omega-3 fatty acids should be started ideally three months before your first attempt.
Skipping the second insemination — Attempting insemination only once per cycle significantly reduces your cumulative success rate. Two timed inseminations per cycle — spaced 12 to 24 hours apart — is the standard recommendation.
At Home Insemination Kit vs. Clinical IUI — Understanding the Difference
A common point of confusion is the relationship between at home insemination and clinical intrauterine insemination (IUI). They are related but meaningfully different procedures.
In clinical IUI, sperm is washed and prepared in a laboratory to remove seminal fluid and concentrate the highest-quality, most motile sperm. The prepared sample is then injected directly into the uterus through a thin catheter — bypassing the cervix entirely. This reduces the filtering effect of the cervix and places sperm closer to the fallopian tubes.
Artificial insemination at home using an ICI kit deposits unwashed sperm into the vaginal canal, near the cervical opening. The sperm must then travel through the cervix naturally. This means more sperm is filtered out along the way, which is why per-cycle success rates for home ICI are somewhat lower than clinical IUI per cycle.
However, the gap is smaller than most people expect, particularly when ovulation timing is accurate and the insemination is performed twice per cycle. Clinical IUI also involves laboratory fees, specialist consultation costs, and clinical scheduling constraints that at home insemination kit completely avoids. For couples or individuals with no significant underlying fertility issues, the intracervical at home insemination kit represents a genuinely cost-effective first approach before advancing to clinical interventions.
The cost difference is substantial. A single cycle of clinical IUI typically ranges from several hundred to over a thousand dollars depending on location and whether ovarian stimulation is included. A complete at home insemination kit costs significantly less, and multiple cycles can be completed for a fraction of clinical costs.
Preparing Your Body Before Using an At Home Insemination Kit
Physical preparation before beginning artificial at home insemination kit is often underestimated. The months leading up to your first attempt matter enormously.
Start prenatal vitamins at least three months before your first cycle. Folic acid is particularly critical for neural tube development and is recommended before conception occurs, not just after pregnancy is confirmed. Vitamin D, omega-3 fatty acids, and iron all support reproductive health and overall cycle regularity.
Maintain a balanced diet and avoid excessive alcohol consumption in the weeks surrounding insemination attempts. Nicotine from cigarettes has a well-documented negative impact on egg quality and implantation rates. Caffeine should be moderated rather than eliminated for most people, though consult your healthcare provider for personalized guidance.
Manage stress actively. Chronic stress disrupts the hormonal balance that regulates ovulation. Yoga, walking, adequate sleep, and mindfulness practices are all practical tools that support hormonal health without the recovery demands of high-intensity exercise.
When to Consult a Fertility Specialist
An at home insemination kit is an excellent starting point, but it is important to recognize when professional guidance will genuinely improve your outcomes.
If you have not conceived after six to twelve well-timed cycles, a reproductive specialist can evaluate whether an underlying condition is affecting your success. Common conditions that make home insemination less effective include polycystic ovary syndrome (PCOS), endometriosis, blocked fallopian tubes, and significant male-factor infertility beyond mild low sperm count.
Women over 35 who have not conceived after six cycles should seek specialist input rather than continuing indefinitely with home insemination, as age-related declines in egg quality and ovarian reserve may require more targeted interventions.
A consultation does not mean committing to expensive treatment. It often means getting a baseline fertility assessment that helps you make a more informed decision about whether to continue with home methods, progress to clinical IUI, or explore other pathways.
Frequently Asked Questions About At Home Insemination Kits
Does home insemination really work? Yes. Research shows success rates of 10% to 20% per cycle for women under 35, with cumulative rates exceeding 40% over multiple cycles when timing is accurate and the process is performed correctly.
How many times should you try home insemination before giving up? Most fertility guidance recommends trying for six to twelve cycles before seeking a specialist evaluation. The odds compound over time, and many people who conceive do so between cycles three and six.
What is the success rate of home insemination with frozen donor sperm? Per-cycle rates with frozen donor sperm are slightly lower than with fresh sperm due to the reduced viability window after thawing. However, frozen donor sperm from a licensed bank is extensively screened for quality and remains a highly viable option across multiple cycles.
Can you do home insemination with frozen sperm? Yes. Frozen donor sperm thawed according to bank-specific instructions works effectively with a home insemination kit. Use the sample within the timeframe specified and inseminate as promptly as possible after thawing.
How do you track ovulation for home insemination? Ovulation predictor kits detecting your LH surge are the most accurate and accessible method. Combine OPK testing with cervical mucus monitoring for the most reliable fertile window identification.
What should I avoid before home insemination? Avoid standard lubricants toxic to sperm, strenuous physical activity, alcohol, smoking, and ejaculation by the male partner within one day before collection. Keep the insemination environment clean and sterile.
How long should I lie down after insemination? Remain lying on your back with hips elevated for at least 20 to 30 minutes after depositing the sample. This gives sperm the best chance of traveling toward the cervix without leaking.
Is an at home insemination kit safe to use? Yes, when using a purpose-built, FDA-cleared kit made from medical-grade materials. Intracervical insemination does not penetrate beyond the vaginal canal and carries no infection risks when performed with sterile equipment.
What does an at home insemination kit contain? A standard kit includes a sterile insemination syringe, a sperm collection cup, ovulation predictor strips, sometimes a cervical disc or sperm-friendly lubricant, and step-by-step instructions.
When is the best time to do home insemination after an LH surge? The optimal window is within 12 to 24 hours of your first positive OPK result. Inseminating once at the positive result and again 12 to 24 hours later gives you the highest probability of sperm being present when the egg is released.
Final Thoughts
An at home insemination kit places a genuinely effective reproductive option directly in your hands — one that respects your privacy, works around your schedule, and removes the sterile, clinical pressure that makes fertility treatment emotionally exhausting for so many people. It is not a shortcut or a workaround. For millions of people, it is simply the right fit — a thoughtful, practical, and scientifically grounded approach to conception.
Success with home insemination comes down to preparation, timing, consistency, and realistic expectations. Master your ovulation tracking, use a quality FDA-cleared kit, inseminate twice per cycle during your fertile window, and give your body the nutritional foundation it needs. And when the data tells you it is time to seek additional help, do not hesitate — a specialist consultation is not a failure, it is just the next informed step.
The path to parenthood looks different for everyone. Whatever that path looks like for you, the right information makes it less overwhelming — and that is always the most important place to start.







Leave a Reply